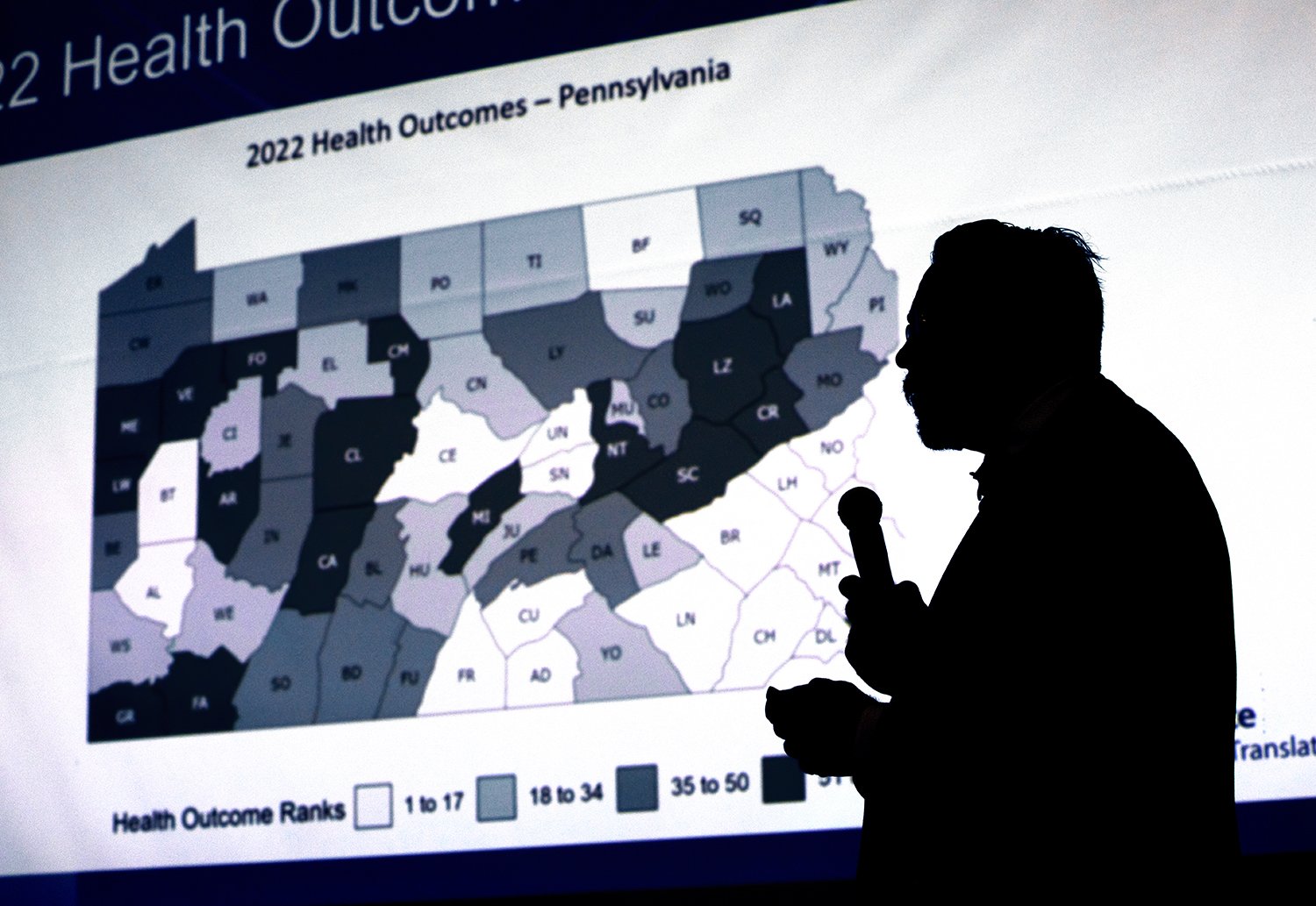
With 95% of Pennsylvanians living within 30 minutes of a Penn State Campus, Penn State Clinical and Translational Science Institute (CTSI) is uniquely positioned to address residents’ psychological and physical health in rural commonwealth communities.
As one of a handful of CTSA (Clinical and Translational Science Award) programs with a rural focus, Penn State CTSI’s mission is to foster collaborative research and provide the necessary tools and resources to help new or proven discoveries reach the people who need it most.
Penn State CTSI offers research support, tools and resources, consultative services, funding, training and education. These efforts foster collaborations across disciplines to translate new discoveries into practice; connect basic and clinical scientists in the discovery of new treatments, procedures and ways to predict, prevent and treat disease; train new and existing health professionals and investigators; and to support research across the continuum, at all Penn State campuses, and for researchers at every stage of their learning and career.
Organizations Involved:
Penn State University
Penn State College of Medicine
Primary Health Network
Allegheny Health Network


-
- Community-Engaged Research Faculty Fellowship Program
- Implementation Science Faculty Fellowship Program
- Early-Stage Investigator Training Program (KL2)
- Graduate Student Training Program (TL1)
- Medical/Graduate Student Summer Program (TSF)
-
- Community and Collaboration
- Research Methods
- Informatics
- Translational Endeavors
- Hub Capacity
- Network Capacity
-
Principal Investigator: Jennifer Kraschnewski, MD MPH
Administrative Lead: Erica Francis, MS
Contact: ctsi@psu.edu
Translational Science in Action:
Scaling Evidence-Based
Interventions Within a Health
System to Achieve Population
Health Benefits
» Translational Research Barrier:The business model of implementing evidence-based programs is poorly understood at Penn State Health, the partner healthcare system to Penn State University.
» Translational Science Innovation: Best practices learned through program implementation process in clinical setting:
1.Have a clear vision and communicate the long-term benefit of the program.
2.Have a framework in place for communication and accountability.
3.Have defined resource planning and appropriate staff time allocation.
4.Have a financial motivation or incentive for the organization to help make the program sustainable.
5.Incorporate programs more seamlessly into the clinical workflow.
» Benefit / generalizability: These findings can be applicable to other healthcare systems and is disease agnostic. They can be applicable to any project aiming to integrate evidence-based programs into a clinical setting, a challenge that is often faced by researchers in the T3 phase of translational research.
» Publications: Segel, J.E., Ortiz, O. E., Shaw, B. W., Stephens, M. B. & Scanlon, D. P. (2019). Becoming a learning health system: Designing and implementing a patient-centered clinical intervention. Management in Healthcare, 3(4), 302-316. https://hstalks.com/article/3798/becoming-a-learning-health-system-designing-and-im/



Dennis Scanlon, PhD
Distinguished Professor,
Health Policy and Administration
Penn State University